HHSC often posts updates in the following sites. We are including this here for your easy access:
https://pfd.hhs.texas.gov/pfd-supplemental-payments-information
Provider Finance Communications | Provider Finance Department (texas.gov)
CMS Lets Jan. 2021 10-year Texas Waiver Stand: Notified Texas that it will drop court action and not rescind the waiver approval. This action protects negotiated budget neutrality and the Uncompensated Care Pool for the 10 years of the waiver (including pool resizing – see below) and enables funding for Directed Payment Programs (DPP) (like CHIRP, TIPPS, etc.) pending CMS approval of annual DPP State Plan Amendments.
Not Rescinding 2022 4 22 Letter to TX
Directed Payment Programs | Texas Health and Human Services
The 1115 waiver approved in January 2021 included a resizing of the UC pool to start in DY 12 and an additional resizing in 2027. HHSC provided CMS with a proposed resizing amount of $4.5B in October 2021 and CMS has yet to approve.
HHSC Resizing Letter:
https://pfd.hhs.texas.gov/sites/rad/files/documents/pfc/pfd-letter-to-cms-1115-waiver.pdf
Resizing Proposed Amount and Calculations:
https://pfd.hhs.texas.gov/sites/rad/files/documents/pfc/dy12-uc-size-template.pdf
BUDGET NEUTRALITY
History – Here’s the famous CMS Budget Neutrality Powerpoint:
CMS Budget Neutrality _EF May 2016 Member Infographics End of Session
THOT UPDATES ON WAIVER COMMUNICATIONS: CMS & HHSC
Late Friday March 11, 2022, after a hearing on Wednesday, March 9, Judge Campbell Barker issued an opinion and order on enforcement of the preliminary injunction requiring CMS to promptly issue a final decision on the remaining DPP programs (CHIRP, TIPPS, and RAPPS). CMS has 14 calendar days (March 25th) to issue a decision on the DPPs.
On the statutory and regulatory framework on the hold harmless guarantees (remaining LPPF issue), the court did not see a need to resolve the interpretative dispute at this time but noted it was legal in nature and was CMS’ final objection to approving the remaining DPPs. Texas agreed at the hearing that it would prefer a final decision on DPPs approval as opposed to continued agency delay. See the ruling here:
State_of_Texas_et_al_v_Brooks-LaSure_et_al__txedce-21-00191__0097.0
DECEMBER 8, 2021: HHSC Responds to CMS’: Waiver Q&A Series
DECEMBER 3: CMS Responds to HHSC Q&A: https://www.hhs.texas.gov/sites/default/files/documents/cms-round-6-feedback-120321.pdf
THOT Summary of CMS’ December 3 feedback to Texas:
https://thotonline.org/wp-content/uploads/2021/12/CMS-Response-12.3.21.pdf
NOVEMBER 15, 2021: CMS Responds to Texas HHSC reiterating offers; citing LPPF issues; and approving BH UC Pool and QIPP programs.
NOVEMBER 3, 2021: Texas on Nov. 2, filed the following motion to enforce the preliminary injunction arguing that CMS is not negotiating in good faith on the proposed programs and funding; and that delays are harming Texas’ health system, providers and patients:
SEPTEMBER 17th UPDATE
HHSC updated DPP preprints based on ongoing work with CMS. This includes limiting CHIRP payments to 90% cap based on hospital class and SDA. This adjustment brings the requested CHIRP funding down to $4.7 Billion dollars. See the link below for the Q and A from HHSC in response to CMS.
texas-responses-to-cms-round-two-feedback 9.20.21
SEPTEMBER 7 UPDATE
HHSC counters CMS’ offer, will implement additional year of DSRIP ($2.49B); as well as UHRIP ($3.3B) using 2021 approach; and QIPP ($1.1B) in 2021 but CMS must continue negotiations on approving other programs approved in January by CMS. See HHSC Letter here:
See THOT Summary of Sept 7 update here:
September 7 1115 Waiver Update Final
CMS responds 8.20. 2021
HHSC yesterday released the CMS response sent Friday Aug. 20th to HHSC. We’ll review and assess. See the reply at the link below:
https://thotonline.org/wp-content/uploads/2021/08/texas-cms-meeting-08-20-2021.pdf
Waiver, CMS, HHSC and Court Updates from Week of August 16th, 2021:
HHSC responded to CMS’ Options. In its Aug. 16 letter to CMS, Texas tells CMS that CMS failed to provide sufficient information for HHSC to choose either of the two options CMS gave the state. HHSC also says that CMS did not provide, as required by the court, information identifying “specific further modifications required for approval” of the proposed DPPs (or State Directed Programs). Rather, CMS simply provided DSRIP as an option or asked the state to withdraw the DPPs and start again. HHSC also identifies the importance of budget neutrality and declined at that time to choose options 1 or 2.
HHSC letter to CMS:
https://thotonline.org/wp-content/uploads/2021/08/HHSC-letter-to-CMS-20210816-letter-mr-tsai.pdf
On August 20, the US District Court Eastern District order filed grants the state’s motion for a preliminary injunction meaning in effect, the rescission is not effective. “With that injunction of the April 16, 2021 rescission, Texas’ demonstration project … currently remains in effect as it existed on April 15, 2021.” The state’s decision not to choose CMS’ proposed options and the today’s court order (attached) appears to give Texas a pathway to approval of some version of the DPPs in a more timely manner AND couldsecure the budget neutrality as under the originally approved waiver.
Beyond HHSC’s statement shared yesterday, we don’t yet know what actions and plans HHSC has regarding pursuit and implementation of proposed DPPs. However, it’s likely HHSC will pursue those DPPs as anticipated in the waiver in effect before the rescission. Also – the court put CMS on notice that it must move forward in its work with the state in good faith: “If a future dispute arises as to whether defendants are complying with the terms of that demonstration project, the court will undertake to decide if such noncompliance has a nexus to the April 16, 2021 rescission that is enjoined by this order. Any contempt sanctions will require showing such a nexus through persuasive, though not necessarily direct, evidence. Agency foot-dragging in implementing the terms of the demonstration project may be inferred to stem from failure to respect the injunction based on timing f any such noncompliance – whether it occurred or intensified after the rescission or this injunction—and any other relevant evidence.”
Court Order 8.20.2021
___________________________________________
FEDERAL COURT AND CMS WEIGH IN ON TEXAS WAIVER AND Directed Payment Programs Aug 12-13, 2021
Court order and CMS letter found at links below.
On Thursday, the United States District Court in Tyler issued an “Order to Clarify Sanctions Standards” in which the court put CMS on notice that sanctions may be imposed for deviations from the terms and conditions of the Trump-administration approved 1115 extension, which CMS previously represented to the court that they are following.
Specifically, the court asserted that CMS had not provided the state with an anticipated approval, nor did CMS provide the state with information required to make technical or substantive modifications to the proposed DPPs within the timeframes prescribed by CMS’ agreement with the state.
The court gave CMS, 24 hours to respond to HHSC and the court (5 PM Friday), or face possible sanctions as well as injunctive relief for the state.
CMS responded shortly before 5 PM on Friday to HHSC and the court with two options for the state.
Option 1. Essentially the status quo from 2021, including reinstatement of DSRIP, with UHRIP and QIPP amounts at 2021 levels. None of the new DPPs are included in this option.
Option 2. Allows the state to withdraw and resubmit the proposed DPPs, including CHIRP, TIPPS and RAPPS. This would mean that Texas would start FY 2022 without having any of these programs, or even programs from 2021, in place. Also, there is little indication asto CMS’ intent with either the size or composition of the proposed/resubmitted programs.
While Option 1 appears to be the most obvious option for the state in the short term, it carries potential downside for the state, long-term.
As you may recall, one of the primary factors for the state to seek extension of its 1115 waiver, prior to the end of January, was to preserve the reasonable budget neutrality calculation guidance in place at the time. It also allowed Texas to count anticipated DPPs as part of baseline budget neutrality: a position favorable to Texas. The waiver approved in January also allows the state to “rebase” at intervals in order for the waiver to keep pace with the growing needs of the state. There is nothing in Option 1 which indicates that the state will receive reasonable budget neutrality terms for future years in the 1115 waiver.
Court order 8.12.2021:
https://thotonline.org/wp-content/uploads/2021/08/show_temp-1.pdf
CMS Letter to State 8.13.2021
______________________________________________________________________________
Trump Administration Approves Texas Fast Track Extension:
HHSC would like to provide an update on the extension request for the Texas Healthcare Transformation and Quality Improvement 1115 Demonstration Waiver.
Texas Health and Human Services Commission (HHSC) and the Centers for Medicare and Medicaid Services (CMS) have reached an agreement to continue the state’s Medicaid 1115 Demonstration Waiver for the next 10 years. This agreement extends the Texas Healthcare Transformation and Quality Improvement 1115 Demonstration Waiver for the next 10 years and allows the state to continue to provide health care to millions of Texans while continuing the waiver’s original goal to transform the Texas Medicaid program into a more efficient and higher quality program by delivering care through a managed care model. The waiver secures over $11 billion in supplemental or directed-payments annually for Medicaid safety-net funding through September 30, 2030.
While the Delivery System Reform Incentive Payment program is being phased out in September 2021, securing the waiver extension now allows the state to develop and implement directed-payment programs for Medicaid-managed care services to improve quality and access, stabilizing Texas’ health care safety-net while providers are continuing to respond to the ongoing public health pandemic. The waiver allows HHSC to continue existing directed-payment programs, including the Uniform Hospital Rate Increase Program for hospitals and the Quality Incentive Payment Program for nursing facilities, and to implement new or increased directed-payment programs for additional providers as outlined in the state’s DSRIP transition plan. Examples of new directed-payment programs could include funding to hospitals, physicians, rural health clinics, and community behavioral health providers.
In addition, Texas received approval for a new uncompensated care program to help offset costs associated with providing care, including behavioral health, immunizations, chronic disease prevention, and other prevention services, for uninsured individuals. This program, which will provide up to $500 million annually, will begin in the fall of 2021 and provide funding to publicly-owned and-operated community mental health centers, local mental health and behavioral health authorities, local health departments and public health districts. Annual funding amounts are scheduled to be adjusted for 2024 and after based on actual charity care costs.
The waiver also continues the current uncompensated charity care pool to support Texas hospitals and other Medicaid providers, including certain ambulance providers, pharmacies, physician and dental clinics. The extension maintains level funding at $3.87 billion each year for the first and second year of the 10-year agreement. Annual funding amounts are scheduled to be adjusted for 2023 and a
Next Step
Texas Medicaid Stakeholders are invited to join the Texas Health and Human Services Commission (HHSC) on Tuesday, January 19 @ 2 pm for an informational webinar. State Medicaid Director Stephanie Stephens, Chief Financial Officer Trey Wood, and staff will provide a briefing on the extension approval announcement related to Texas’ 1115 Transformation Waiver. Please register at the following link: https://attendee.gotowebinar.com/register/8399929499461176075.
_______________________________________________________
Texas’ Fast Track Extension Request clears first hurdle:
CMS on Dec. 15 determined TX’ request meets requirements for “a complete extension application and is exempt
from the requirements for public notice and comment.” CMS still needs to approve the actual request, but this approval is the first necessary approval in the process. Congrats to HHSC. See letter to Medicaid Director Stephanie Stephens below:
What is a Fast Track Waiver?
In November, 2017, the Trump administration released guidance to minimize burdens and increase efficiency in waiver application and review processes, including the “fast track” option. [See HMA’s discussion of this here: https://www.healthmanagement.com/blog/new-cms-guidelines-expedite-approval-1115-waivers-state-plan-amendments/ ] Generally, section 1115 demonstrations are approved for an initial five-year period and can be extended for up to an additional three to five years, depending on the populations served. States commonly request and receive additional 3-year extension approvals. Certain demonstrations that have had at least one full extension cycle without substantial program changes will be eligible for CMS’ fast track review process for demonstration extensions. https://www.medicaid.gov/federal-policy-guidance/downloads/cib07242015-fast-track.pdf
Budget Neutrality: What is it and why does it matter?
Think of budget neutrality as the amount of funds that CMS allows a state to spend in waiver programs. The amount is negotiated with the federal government based on trended historical Medicaid cost and utilization data. Texas’ first Transformation Waiver included historical hospital Upper Payment Limits funds that otherwise would have been lost in a transition to Medicaid Managed Care. Under pressure to limit federal waiver spending, CMS adopted new guidance to reduce waiver funding (or budget neutrality). Texas’ Third Waiver renewal would be subject to these more stringent limits. See CMS’ guidance here: https://www.medicaid.gov/Federal-Policy-Guidance/downloads/SMD18009.pdf
DSRIP Transition plan:
December 2020 – HHSC released its DSRIP Program Plan laying out a crosswalk of DSRIP funds to Directed Payment Programs and other programs for: Hospitals, Physician Groups, Community Mental Health Centers, & Local Health Departments. HHSC is required to submit the plan to CMS by the end of this year. See HHSC’s powerpoint here:
20201211 DSRIP Partner Engagement Meeting
Waiver Fast-Track Extension:
HHSC quickly created and submitted a request to CMS for a “Fast Track” waiver extension. The request seeks to stabilize Texas’ waiver programs and related healthcare for Texans; including ensuring continued funding availability through the pandemic and recovery. This waiver extension differs technically from a waiver renewal, and is separate from, but not in conflict with the already submitted DSRIP Extension request (see below). Links below are for THOT’s high level summary and HHSC’s request and related documents.
HHSC summary 12.17.2020_revised final
https://hhs.texas.gov/laws-regulations/policies-rules/waivers/waiver-renewal
DSRIP Extension Request:
THOT worked with providers and with other associations to illustrate the impacts to patient services and our delivery system from COVID, asking HHSC to seek a one-year DSRIP extension. The extension would help stabilize services and maintain access to uninsured care in the DSRIP program. Links to HHSC’s Extension Request; the Associations’ Extension Request to HHSC; and a two-page summary of the Associations’ request are below:
HHSC_Texas_DSRIP_Extension_Request-20201016
DSRIP_COVID-19_Explainer-2-Pager_Final
DSRIP Transition plan:
On August 2, HHSC released its draft DSRIP transition plan:
Public comments are due August 15th to HHSC on HHSC’s comment survey: https://www.surveymonkey.com/r/DSRIPTransitionPlan
Texas’ draft DSRIP Transition Plan is due to CMS in October 2019; with a final due five months later in March, 2020. Dell Medical School has been assisting HHSC with development of the draft DSRIP Plan. In November 2018, THOT and other stakeholders submitted proposals for alternative uses of DSRIP funds in response to HHSC’s request. HHSC published those plans in an excel file available on HHSC’s website at: https://hhs.texas.gov/laws-regulations/policies-rules/waivers/medicaid-1115-waiver/waiver-renewal
NEXT UP:
UC 14 – 17 Payment Methodology:
On Aug. 2, 2019, HHSC reiterated that it would announce a plan to determine both the allocation of withheld UC funds and a means of offsetting the UPL obligation. HHSC also noted that it is still deliberating on an appropriate path forward; and will inform stakeholders of its decision as soon as possible. HHSC will attempt to add an amount of funding to the upcoming UHRIP program year to take into account the UPL obligation. While the added funds will not be reflected in the mid-year applications, HHSC will manually add the funds after application submission.
HHSC has been reviewing at least six models for distributing these funds while paying back a debt from year one of the waiver. HHSC’s three models all required significant levels of recoupment from hospitals. THOT proposed an approach to take the payback out of reserved 14-17 funds, and then distribute the remaining amounts with a methodology that state had used in a similar DSH 14-17 payment (Option X). CHAT proposed a model, and Tenet also proposed a model for distribution. All hospitals agree that a no – recoupment approach for paying back CMS with 14-17 funds before distributing remaining amounts (such as THOT proposed) be adopted.
Background: HHSC withheld funds in waiver years 2014 – 2017 in the event a Children’s Hospital lawsuit required that it pay hospitals amounts above CMS’ calculated limits for the DSH program (or Hospital Specific Limits HSLs). The judge in that lawsuit ruled that the Social Security Act language did not support CMS’ interpretation of its HSL calculation. The judge concluded that payments made by commercial insurance for Medicaid enrollees (e.g., NICU children automatically eligible for Medicaid) should not be included (though costs should be included) in the HSL for purposes of setting DSH payment limits. Texas chose to also ignore payments for Texas Medicaid enrollees in the calculations of programs like DSH and the waiver Uncompensated Care program, shifting significant funding in these programs from providers with more unfunded patients, to providers with patients having multiple payment sources. A Congressional Advisory Commission, the Medicaid and CHIP Payment and Access Commission or MACPAC, has issued recommendations to Congress that the Social Security Act be amended to avoid double payments for Medicaid patients and to mitigate related shifting of funding from lower-funded providers. MACPAC recommends that both the payments and the costs of Medicaid patients with other insurance be excluded from consideration in determination of maximum DSH payments to hospitals.
CMS approval of UC Pool Size for 2020-2023.
HHSC anticipates having a final annual pool amount by September 2019. Estimates of $3.8 billion have been used in recent HHSC modeling, but CMS will review hospital cost report data in HCRIS before finalizing any number.
UHRIP
On August 2, 2019, HHSC announced it received CMS approval for providing UHRIP supplemental payments for SFY 2020 (starting September 2019). HHSC had indicated that $1.6 billion is earmarked out of 1115 waiver budget neutrality for these payments. HHSC is also pursuing a simplified supplemental payment program recommended by THOT and based on similar programs in use in Michigan and Tennessee. Under these simplified programs, lump supplemental payments can be made retrospectively to hospitals, improving transparency, reducing advance time and state hold time of IGT match funds, and reducing HMO risk and related risk payments from IGT funded payment programs, HHSC hopes to implement a simplified supplemental UHRIP program in September, 2020 (SFY 2021).
SOCIAL DETERMINANTS OF HEALTH
Texas’ 1115 waiver provided opportunities to address Social Determinants of Health (SDOH) in Texas leveraging our health systems’ close relationships with communities and community based organizations. A growing body of research details the impact SDOH have on health, and healthcare utilization. CMS recently announced a bipartisan proposal called the Social Determinants of Health Accelerator Act that will provide grants of up to $25 million to “help states and communities devise strategies to better leverage existing programs and authorities to improve the health and well-being of those participating in Medicaid.” https://www.forbes.com/sites/brucejapsen/2019/07/25/congress-warms-to-paying-for-social-determinants-and-health-industry-cheers/
CMS’ 1115 Rebasing Powerpoint (pdf)
Request for Withdrawal of Waiver Funding Disallowance (pdf)
HHSC 21-Month Extension Request (pdf)
CMS Response to Disallowance Reconsideration Request (pdf)
Testimony
THOT Testimony for House County Affairs Committee Hearing May 16
Background on 1115 Waiver
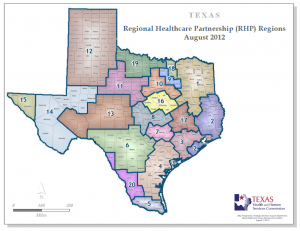
THOT Members have a strong commitment to innovation and healthcare transformation. Our members serve as 9 of the state’s 20 1115 Waiver anchors for the Texas regional healthcare partnerships (RHP).
News Release
Texas Health and Human Services Commission
Chris Traylor
Executive Commissioner
Date: May 2, 2016
Contact: Bryan Black, 512-424-6951
Big Win for Texas, HHSC Receives Extension for 1115 Waiver
AUSTIN – The Health and Human Services Commission and the Centers for Medicare and Medicaid Services have agreed to extend a state and federal partnership that finds innovative ways to deliver healthcare.
The 1115 Waiver, which funds Uncompensated Care and the Delivery System Reform Incentive Payment Program (DSRIP), was extended 15 months under an agreement between the health agency and CMS. The agreement will take the program through December 2017 and will maintain its current funding.
“We’re pleased these innovative programs will have the opportunity to continue,” HHS Executive Commissioner Chris Traylor said. “These programs are improving health care for Texas’ Medicaid clients and creating cost-savings for taxpayers.”
Over the next 15 months, HHSC and CMS, which oversees the Medicaid program, will continue negotiating a longer term extension.
DSRIP consists of local programs working to improve health care delivery costs and outcomes.
There are 1,451 DSRIP projects across 20 regions in the state. In each region a coalition of governments, hospitals and other providers are charged with coming up with novel solutions to containing health care costs while preserving access and quality. Most projects focus on increasing primary and preventative care, which not only improves outcomes, but saves money by reducing the need for expensive emergency room visits. The waiver program also helps hospitals with uncompensated care costs.
One program in Travis County trains paramedics to visit people who have frequent emergency room visits. The program has found some people can’t treat conditions such as diabetes because they don’t have a ride to pick up the materials. Helping prevent serious episodes is healthier and cheaper than an emergency room visit.
“One of the things I like best about these projects is they use the knowledge of the people on the ground to identify their problems,” Commissioner Traylor said. “Beaumont faces different issues than El Paso and the waiver program takes advantage of local expertise.”
The Uncompensated Care program and Delivery System Reform Incentive Payment programs are funded through a combination of federal and local money. Both Uncompensated Care and DSRIP contribute $3.1 billion a year, each.
Success Stories
There are strong success stories found across the state. Please click below for a few of these stories:
University of Texas Medical Branch Story of Hope
Childress Regional Medical Center
Parkland Post-Partum Mental Health Initiative
Central Health: Austin Travis County Integral Care Mobile Crisis Outreach Team
Waiver Programs
Please click on the links below to learn more about the waiver programs, regional plans, successful projects, and more.
THOT members serving as anchors are listed in bold.
RHP 1, Anchor: UT Health Northeast, Website: http://www.uthealth.org/waiver/
RHP 2, Anchor: University of Texas Medical Branch, Website: http://www.utmb.edu/1115
RHP 3, Anchor: Harris Health System, Website: http://www.setexasrhp.com/
RHP 4, Anchor: Nueces County Hospital District, Website: nchdcc.org/1115-waiver-information.cfm
RHP 5, Anchor: Hidalgo County, Website: www.southtexasrhp.com
RHP 6, Anchor: University Health System, Website: texasrhp6.com
RHP 7, Anchor: Central Health, Website: texasregion7rhp.net
RHP 8, Anchor: Texas A&M Health Science Center, Website: tamhsc.edu/1115-waiver/rhp8.html
RHP 9, Anchor: Parkland Health and Hospital System, Website: http://www.texasrhp9.com
RHP 10, Anchor: JPS Health Network, Website: http://www.rhp10txwaiver.com/
RHP 11, Anchor: Palo Pinto General Hospital District, Website: texasrhp11.com
RHP 12, Anchor: UMC Health System in Lubbock, Website: texasrhp12.com
RHP 13, Anchor: McCulloch County Hospital District, Website: texasrhp13.com
RHP 14, Anchor: Medical Center Health System, Website: http://www.texasrhp14.com/
RHP 15, Anchor: University Medical Center of El Paso, Website: umcelpaso.org
RHP 16, Anchor: Coryell County Memorial Hospital Authority, Website: texasrhp16.com
RHP 17, Anchor: Texas A&M Health Science Center, Website: http://www.tamhsc.edu/1115-waiver/rhp17/index.html
RHP 18, Anchor: Collin County, Website: http://www.tx-rhp18.net/home
RHP 19, Anchor: Electra Memorial Hospital, Website: http://texasrhp19.com/
RHP 20, Anchor: Webb County, Website: http://www.webbcountytx.gov/IndigentHealthCare/HealthcarePartnership/
Primary Contact Information for Anchors by Region